Why The US Healthcare Care System Costs So Much – Part Three – Overtreatment
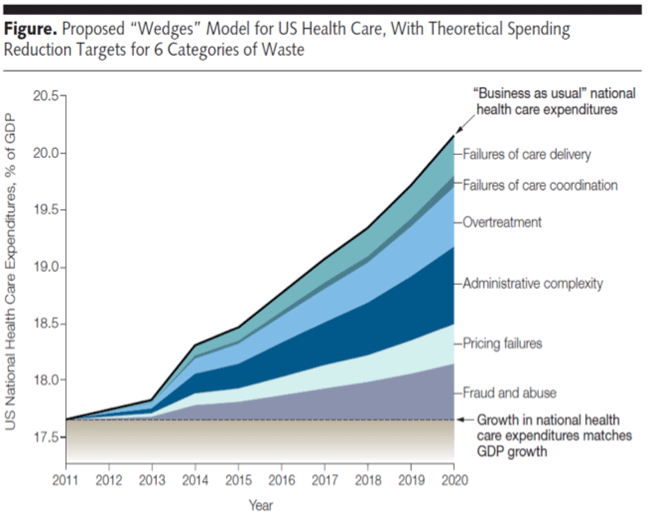
This post is about overtreatment, one of the waste factors driving health care costs in the U.S. (Eliminating Waste in US Health Care, Berwick and Hackbarth, JAMA, 2012).
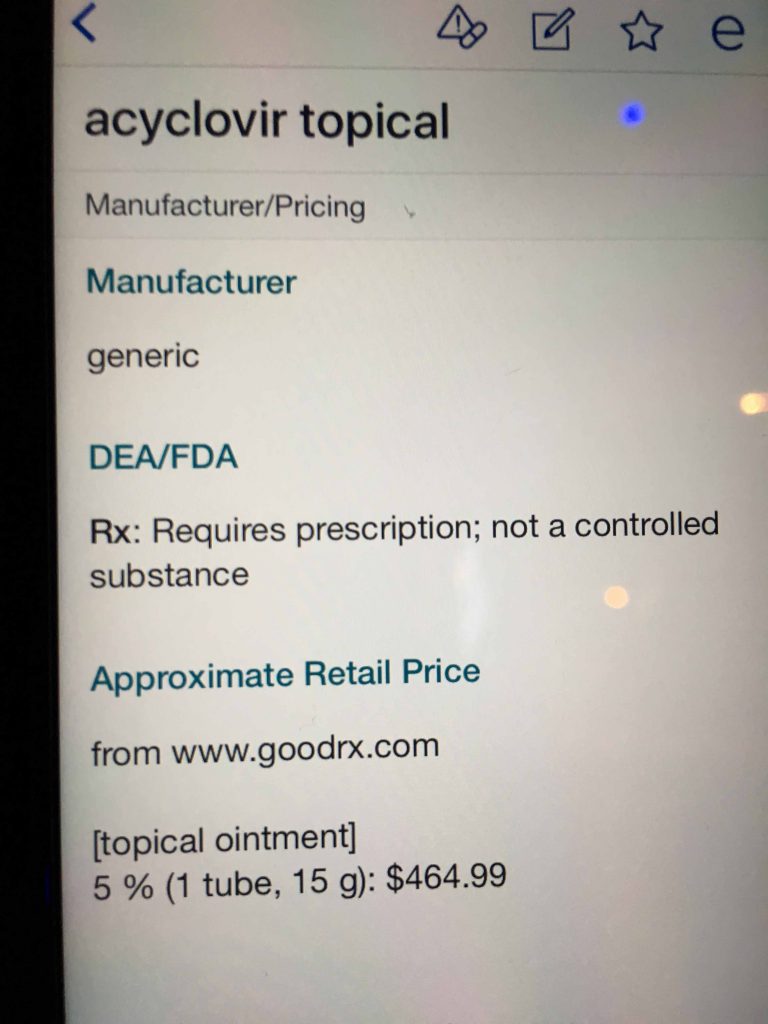
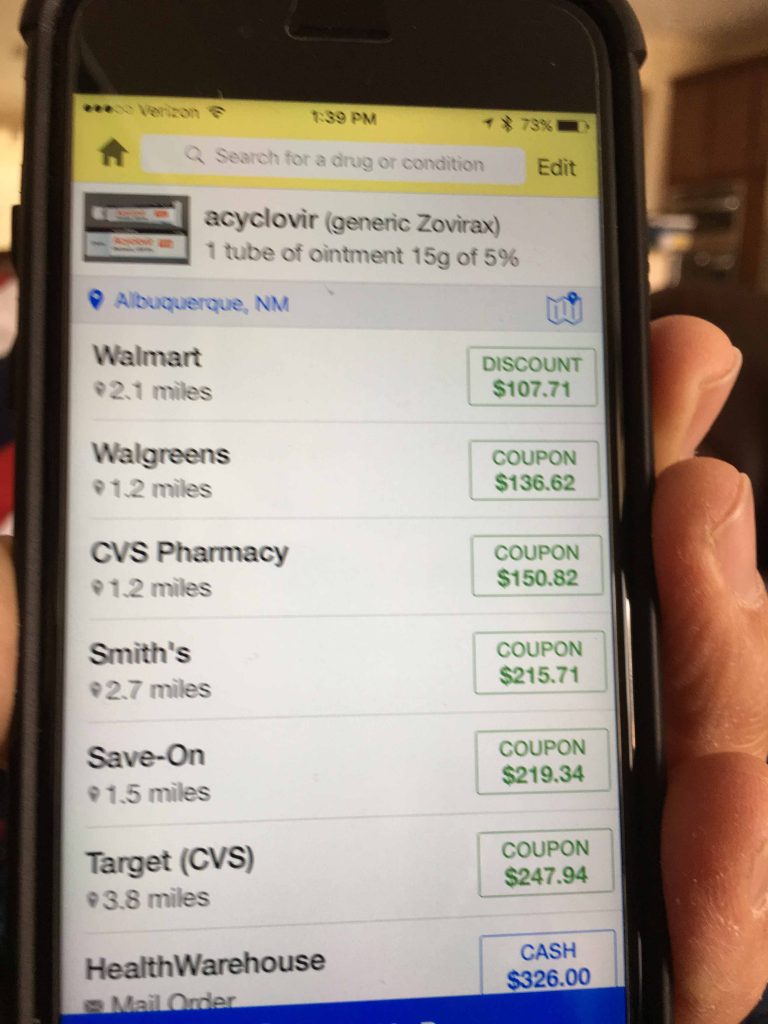
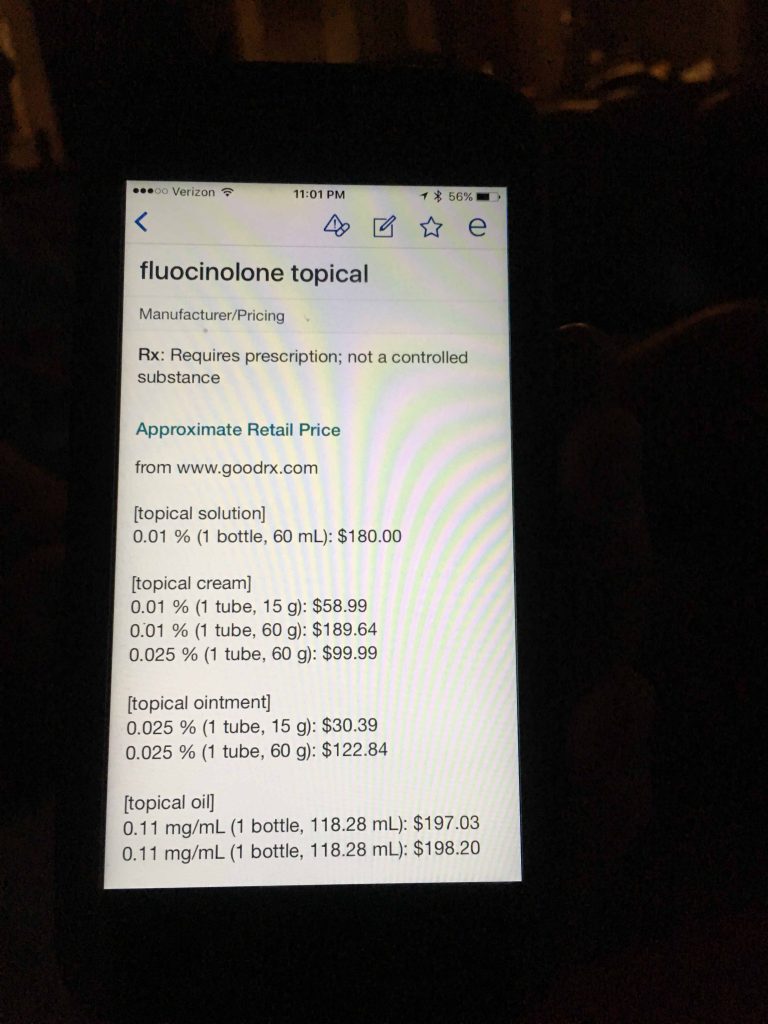
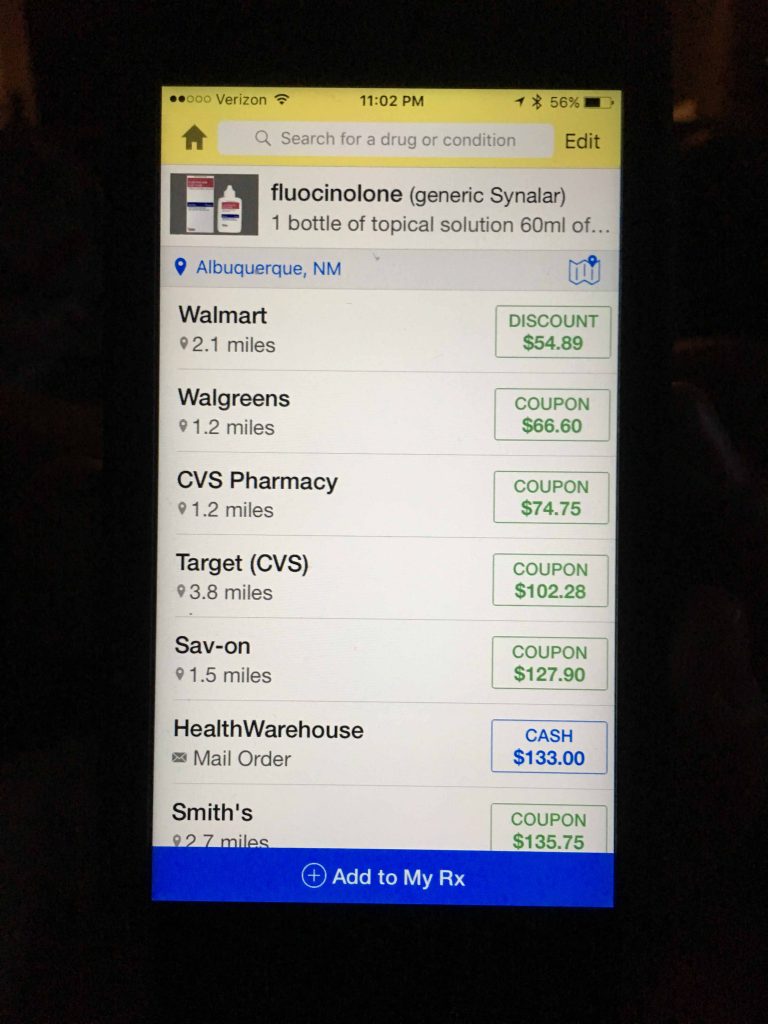
Berwick and Hackbarth define overtreatment as: “the waste that comes from subjecting patients to care that, according to sound science and the patients’ own preferences, cannot possibly help them—care rooted in outmoded habits, supply-driven behaviors, and ignoring science. Examples include excessive use of antibiotics, use of surgery when watchful waiting is better, and unwanted intensive care at the end of life for patients who prefer hospice and home care. We estimate that this category represented between $158 billion and $226 billion in wasteful spending in 2011.”
While this statement on the surface is true, the actual subject is way more complicated and complex than this. And, this is not just a USA issue; this is a global problem. You have no idea how many articles I’ve read about this from countries in Europe, China, Australia, India, etc. Just select one subject, like overuse/prescribing of antibiotics. Every country is reporting the same thing and every country is dismayed by the results of efforts to reduce inappropriate antibiotic prescribing. Folks like Berwick and Hackbarth make this seem like a simple thing, that there is science that is so specific that once told to a practitioner, they will stop prescribing inappropriate antibiotics. If that were true, the global reports I just mentioned would have produced fantastic results. That ain’t happened yet!! The administrators, who don’t understand health care, simply say things like, “Those stupid, stubborn practitioners! Why can’t they just get in line with this! They are ignoring the science!!”
Yeah, those stupid people who had to go to college, get excellent grades, pass a stiff entrance exam, learn a ton of stuff, graduate from a post-graduate school like a Medical School, obtain a doctorate level degree and spend 3-5 years in on the job training before going out in the world to practice! Why can’t they just get in line!! This, is spoken by guys with Bachelor’s degrees or maybe a Masters degree that has no clinical content and they have no clinical experience. Especially those Finance guys who have all the power and who are never and have never been in an exam room with a patient!
But, I’m not bitter about it….
In the land of truthsabouthealthcare.com, here are some of the major categories driving overtreatment.
- Practitioners are taught their utilization behaviors while in training. There has been literature out there for about 20 years showing where a physician trained creates long lasting impact on what they order and how they take care of patients. Even when a physician moves away from where they were trained, their academic center’s utilization pattern persists.
- Practitioners are influenced by their peers and the specialists in their region. Jack Wennberg, MD from Dartmouth (the originator of the Dartmouth Atlas) saw this with his first small area analyses in the 1970’s where the rate of procedures in one state were drastically different from another state without a difference in burden of illness in the population. Sometimes only one county in a state drove the over treatment statistics for the entire state.
I can personally attest to these first two factors. These first two can actually drive underutilization as well, so I am going to include stories about both over and under-treatment. Here are the stories.
I trained at a very prestigious Medical School and Training center in the last half of the 1970’s/first half 1980’s. There were two things that were “banged into our heads” related to two chronic conditions that, we were taught, were best practices: 1. Following a diabetic person’s A1c level 4 times a year, especially if their disease wasn’t controlled, and 2. Any asthmatic person who used more than one rescue inhaler (albuterol) a month must be prescribed a controller inhaler (at the time only corticosteroid inhalers were available).
So, for every diabetic in my practice, they got A1c’s on a regular basis and I would only prescribe a new or “problem” asthmatic one month’s supply of a rescue inhaler (until I knew them to be trustworthy) so I could keep track of how often they needed a refill. If it was less than a month, I put them on a steroid inhaler.
I graduated training in 1982.
In 1993, I became the Medical Director of a Physician Group Practice in New York. I was at a monthly Internal Medicine meeting and had some data showing that their diabetic population’s blood sugars were not well controlled and they had a paucity of orders or completed blood tests for A1c’s for these patients. To the one, they said that an A1c was a useless test to the point that one Internist actually pounded his fist on the table saying he wouldn’t order a useless test. I had to recruit an endocrinologist and collect a pile of medical literature articles to convince them to start ordering the test.
In 1996, I took over a practice in the same area in New York that had only consisted of two physicians assistants (PA) who were supervised by a hospital’s emergency department physicians who never went to the PA’s offices to see patients or even talk to the PAs except over the phone. Their diabetics were not well controlled. They had never ordered an A1c. When I asked them why, they said the ER physicians told them it was a useless test. Same region, same perception.
Getting A1c’s is a standard of care for diabetic patients…look it up.
So, here, the regional perception resulted in underutilization that resulted in undertreated patients resulting in increased complications and, likely, higher medical costs.
Here’s the asthma story. I told you above how I managed asthmatic patients. I hardly, if ever, had one of my asthma patients present to the emergency room with a bad asthma attack. I had the moderate to severe patients on steroid inhalers, I had nebulizers in my office, I had IV steroids in my office. I saw them in my office if they had an exacerbation, and treated them there, which wasn’t often. This was how I was taught to treat asthma in the late 1970’s, early 1980’s.
In the mid-1990’s, asthma care began to emerge as a problem, the most notable issue being patients weren’t being put on controller meds (i.e., steroid inhalers) when they should be. They were being managed with rescue inhalers only, i.e., overusing rescue inhalers. This sparked a nation-wide effort to improve the use of controller meds in asthmatics. Health Plans adopted Asthma Programs, hired Disease Management companies, etc. Lots of dollars spent on this. This surprised me because of the intensity of the messaging we got in training (where I trained) about putting people on controller meds.
It’s 1996. I’m in that practice with the two PA’s. I was on “service call” (you know, when we old docs were still admitting our patients to hospitals and had to “pay back” the hospital by taking patients whose doctors didn’t admit to that hospital or were unavailable, like they were on vacation and didn’t have a call group to cover for them or they were ambulatory only physicians). I got called to the ER for a patient who was having a serious asthma attack. And, boy, was she! She was a 20 year old, really bad blood gases (O2, CO2 in her blood), had a fever, elevated white blood cell count. She was so sick I had to admit her to the ICU (which had no Intensivists, you had to take care of your own ICU patients). She tested positive for Legionnaires disease.
As part of my admission history and physical exam, I did as detailed an asthma history as possible. Her story was terrible. She, for several years, had been home bound because of severe shortness of breath. She had never been on a controller medication, only a rescue inhaler (albuterol). She had never had oral steroids prescribed for her. Basically, she was a severe asthmatic on minimal medical treatment but over using albuterol, multiple inhalers a month.
I managed her for almost a week in the hospital and discharged her on a pulse of oral steroids, then a steroid inhaler and her rescue inhaler. I saw her in follow-up frequently at first, then spaced out her appointments because she was doing well. At her six-month visit, she and her mother came in in together. They were astonished by the fact that this young woman was now leading a normal life, going out doing whatever she wanted, never short of breath. They thought it was a miracle. It wasn’t, it was maintaining the proper treatment.
This was 14 years after I graduated training. Again, a net under-treatment (she was being over-treated with albuterol), but the phenomenon is the same for over-treatment. This was a national problem that should have been solved in 1980. Weren’t any other medical training centers banging this treatment protocol into physicians’ heads? Was my academic center an outlier? It seemed odd to me.
Here’s an example of regional overtreatment.
Between 1990 and 1993, I was in a Medical Group in Minnesota. They were capitated (paid a lump sum per patients per month instead of a fee for each service). Anytime I wanted one of my patients to have a cardiac stress test, I had to fill out a requisition that included why I thought the patient needed a stress test. If the cardiologist couldn’t align my thinking with the cardiology guidelines for the test I ordered, he would call me for clarification. If we agreed with the indication, the patient got the test. If not, we agreed on the right course of action according to guidelines and the specifics of the case. This was especially true for Thallium (radionuclide) stress tests where a patient got an injection of a radioactive material that would be imaged with a scanner. We did very few Thallium stress tests in Minnesota, as getting a Thallium stress test had more specific indications that a “standard” stress test (the exercise part only).
I moved to New York. The cardiologists in the region where I practiced were advising that every stress test candidate should get a radionuclide stress test, a standard stress test wasn’t good enough. They used sestamibi (Technetium-99), a similar radioactive material to Thallium. Additionally, they wouldn’t do the test unless the patient came to their office for a pre-stress test cardiology evaluation and the patient had to also have a post-stress test visit to go over the results (which were already reported in a paper report, like an X-ray report, with the cardiologists interpretation). It would be like a radiologist wanting a pre-chest X-ray or pre-CT-scan visit and a post-chest-X-ray or post-CT-scan visit for every Chest X-ray and CT-scan they did. Imagine the costs for this. And totally unnecessary.
Well, these patients were being dramatically over-treated! And the costs were incredibly high for stress tests in that region, because they convinced all the PCPs that this was the best treatment for their patients. Did I mention that the cardiologists owned the sestamibi scanner? And PCPs are often unwilling to challenge a specialist. I actually had a PCP tell me he did whatever a specialist told him to do with patients because he could never challenge a specialist since the specialist knew more about their specialty than he would ever know. My philosophy was, it was my job as a PCP to make sure specialists were following their own specialty’s guidelines. You have no idea how many times I cought a specialist not following his/her own specialties guidelines. More on this later.
The science isn’t as scientific as it looks. There are lots of reasons why I’m saying this and I’ll have to defer a real deep dive into this in later posts. Here are a couple of quick hits about it:
About every 10 years, some PhD-type does an analysis of the medical literature for validity. Generally speaking, their conclusion is about 70% of articles don’t prove (or disprove) what they say they are proving. First you have to sift out any article that is sponsored by a drug or device company. This is because a drug or device company sponsored article never shows a neutral or negative result. They suppress those articles and only publish articles with positive results, even if the research is terrible, which it often is. They will actually stop the research if the preliminary results are negative. Secondly, most studies are flawed. When researchers do what is called a “meta-analysis” (this is where a researcher gathers all of the articles on a subject and tries to see if they can statistically prove whether something works or not) a common conclusion is, there is no valid result or recommendation because the research on the subject is so bad, even combining their data doesn’t actually prove whatever it is studying does anything. Either the statistics are bad, the study design is flawed, or the study didn’t have enough “power” (e.g., not enough patients in the study to reach statistical significance), etc.
For example here’s an except from a recently published meta-analysis on reducing opioid use:
“Limitation: Heterogeneous interventions and outcome measures; poor-quality studies with uncontrolled designs.
Conclusion: Very low quality evidence suggests that several types of interventions may be effective to reduce or discontinue LTOT and that pain, function, and quality of life may improve with opioid dose reduction.”
Unfortunately, the media, not knowing anything about study design or biostatistics, reports to the public the results of these flawed articles that actually prove nothing and people panic over them.
What is “proven” today, gets “disproven” several years later. Often, it’s a 180 degree turnaround. Here are two examples:
Estrogen/progesterone therapy for post-menopausal women (HRT; Hormone Replacement Therapy). In the 1990’s “the studies” showed that every post-menopausal women should be on estrogen (and progesterone if they had a uterus) because it prevented breast cancer, heart disease and strokes. Some folks considered it malpractice to not prescribe HRT. In 2002, a large study came to the exact opposite conclusion (and all studies since). HRT caused heart attacks, strokes, blood clots and breast cancer. Suddenly, it was considered to be malpractice to prescribe HRT!!
I can’t tell you how many women to whom I prescribed HRT in the 1990’s. I’m always wondering if that act killed any of them. Statistically, it must have. It is horrifying for a physician to think he or she has killed someone!
Here’s another one.
High dose chemotherapy with bone marrow transplantation for metastatic breast cancer (HDC/BMT). The first studies, around 1990, were accepted by the oncology specialists and they started promoting the procedure. Health plans looking at the research on this concluded that the research wasn’t strong enough to consider the treatment to be not experimental, and began denying the treatment (I was a Medical Director in a health plan that really looked at these studies and concluded the evidence wasn’t strong enough to say the treatment should be mainstreamed). The estate of a woman who died of metastatic breast cancer after HDC/BMT, whose insurance coverage for the treatment was denied by her health plan, sued the health plan and won. Massachusetts, New Hampshire, Virginia, and Minnesota mandated insurance coverage for HDC/BMT based on the court cases (not the clinical research). In 1999, a series of research studies showed that women were dying more from the HDC/BMT than “conventional therapy” and the outcomes were no better. So, the four states mandating coverage were actually party to killing women unnecessarily. Interestingly, no one sued them. The new research prompted review of the initial studies and the conclusion was some of the data was fabricated. Yes, fraudulent! And laws were passed forcing insurers to approve them!! And all of those oncologists just went along with it, not fully looking into the validity of the articles to be sure they were proving the treatment was beneficial. It was like everyone was mass hypnotized! Except the health plans…
To show you how some specialists never give up on a treatment they became invested in, in 1999 I was a Medical Director for an HMO in Michigan. Two months after the new research discrediting the HDC/BMT treatment, I got a request from the University of Michigan to approve a “tandem” HDC/BMT for a woman with metastatic breast cancer. A tandem HDC/BMT is when you do two in a row. Given the recent revelations about HDC/BMT, I denied the request. The U of M requested an expedited appeal to the state HMO review board using the argument that just because one HDC/BMT killed women more than usual care without better outcomes, you couldn’t say doing two in a row wouldn’t be better (really, this was their argument!). In Michigan, when an appeal is expedited, the board chooses several physicians from the specialty within which the procedure resides, in this case oncologists, to determine if the denial should be overturned or not. The expedited appeals panel of oncologists overturned my denial and we had to cover this highly experimental and likely dangerous procedure!!
No one does HDC/BMT for breast cancer anymore! Are you still wondering why physicians are wary of the “science”? Oncologists killed dozens of women based on poor science.
Here’s a link to a recent Perspective article in JAMA Internal Medicine about the same thing related to PSA testing (“No Wonder No One Trusts Us”; JAMA Internal Medicine, July 24, 2017). The physician author describes trying to explain to his 20 year patient that the guidelines for PSA testing have changed…again!
http://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2645148?utm_medium=alert&utm_source=JAMA%20Intern%20MedPublishAheadofPrint&utm_campaign=24-07-2017
“Science” equals “Guidelines”. Specialty societies publish guidelines, which are interpreted by folks like Berwick and Hackbarth to be “the science”. The truth is, only about 20% of guidelines have any basis in science (because of the reasons above). The remaining 80% is tantamount to “expert opinion”, which is based on a physician’s experience and personal interpretation of the available literature. It is inherently biased. Plus, a significant (up to 80% depending on the specialty) of the physicians on the specialty committees promulgating the guidelines have financial ties to drug and device companies. Another huge bias.
I actually had a physician who was on a specialty guideline committee tell me that one of the major elements of the guideline was passed (even though the majority of the committee said there was no evidence supporting it) because one physician on the committee badgered each committee member so much (including at meals, on breaks, etc.) that they included it just to get him off their backs!!
So, physicians will say they know as much as “those guys on the committees” and they have their own “expert opinion” which is just as good. When I was in Ann Arbor Michigan, I had specialists tell me the recently released guidelines by their own specialty were wrong, that they knew better than their own Specialty’s guideline committee and would be treating patients differently from the guidelines. To my face!
Patients’ cases aren’t cut and dried. The pundits, administrators and finance folks think dealing with patients is like dealing with spreadsheets. They also don’t see the variation in patient presentation that deviates from the cleaner presentations in guidelines and research articles.
For example, one of the first things in a clinical research article is the “patient exclusions”. They exclude so many patients they end up with a very narrow stripe of the population. It’s like a “pure” population that only exists in research studies.The expectation is, you then apply the recommendations (based on this pure narrow stripe) to all patients. Doesn’t that seem odd to you? Check out this article to see what I mean; “Injurious Falls and Syncope in Older Community-DwellingAdults Meeting Inclusion Criteria for SPRINT”, JAMA Internal Medicine Published online July 17, 2017. The community dwelling population had five times the falls and syncope than the SPRINT study population. In addition, the results are based on the average outcome when even this pure population has a bell curve distribution of outcomes.
Here’s how this plays out. Imagine a study trying to prove that a drug reduces blood pressure. On the right side of the bell curve people have no reduction in their blood pressure and they have adverse effects (meaning a non-blood pressure related adverse effect like nausea or a rash). On the left side of the bell curve people have big reductions in their blood pressure and little adverse effects. At the middle of the bell curve (the average) there is a modest reduction in blood pressure and a modest number of adverse effects. The drug gets approved. A physician will give the drug to three patients. One has no blood pressure reduction despite dose escalation and has a bad adverse effect, one has what the research reported, modest blood pressure reduction and a minor adverse effect, one will have a terrible drop in blood pressure causing fainting and no adverse effect (you would consider a dose reduction in this patient).
Physicians see the bell curve, not the average, and the end of the bell curve that impacts their memory and behavior the most is the one within which the patients they’ve treated had the failures where patients get hurt, have a bad outcome (even if this happens only once in their practice). So, then, they “err” on the side of mitigating the bad outcome side of the bell curve, i.e., they treat patients assuming they are likely to be on the bad side. They don’t see the adverse effects of their actions, as those are either delayed or require looking at the outcomes of thousands of patients (they only have 1500-2000 people in their panels of which only a fraction have the illness in question).
For example, this is what happens with antibiotic prescribing. All the practitioners know you shouldn’t prescribe antibiotics for a cold, but they do when the presentation isn’t completely classic for a cold (the average presentation). Any additional symptoms signal a potential for a non-viral component to the illness (the bad side of the bell curve) where the patient’s status could worsen and result in a serious infection. And the non-viral components are rarely detectable with a test on the spot, so they can’t prove they were right. So, thinking they are acting in the best interest of the patient with the information at hand, they prescribe an antibiotic (i.e., they are avoiding a serious infection).
It’s easier and faster to do something than persuade a patient they don’t need something. Two things drive this: 1. Practitioners think patients want things even if they don’t ask and, 2. Patients specifically ask for things.
If a physician feels pressured for time, they are tired (or both), or they want to please their patient and not lose patients, they will prescribe things they know they have no good data to support prescribing. I’ve had physicians in medical groups tell me they give the patient what they want because the administrators are yelling at them about their patient satisfaction. One of the largest volume of patient complaints is the doctor didn’t give the patient what they thought they should get. I led a project to reduce antibiotic prescribing for viral illnesses in a medical group and the volume of patient complaints about not getting an antibiotic spiked.
There is actually literature that shows that practitioners prescribe more antibiotics for colds later in their clinic sessions than at the beginning. They “get behind” and they are getting tired and just want the session to end. There is also literature related to the power of patient requests on the behavior of practitioners. This is why drug companies are paying billions for Direct-To-Consumer advertising. The patient comes in asking for the drug. It’s been proven to be an effective strategy.
It is financially beneficial to the practitioner to over-treat. This phenomenon is so well known and prevalent that there are laws about it, the Stark Laws. But the Stark Laws only cover a minority of this problem.
Remember, in the end, it’s all about the money.
There’s a saying in the medical world: Send your patient to a surgeon and you can just about guarantee they will get a surgery, whether they need it or not. Surgeons hate to say you don’t need a surgery. There was actually an opinion article in a prestigious surgery journal appealing to surgeons to NOT do surgery, that saying someone doesn’t need surgery is just as important as doing a surgery. However, this is still really hard for surgeons to do. I’ve talked to dozens of surgeons about this. Their desire is to be in the OR and avoid office hours as much as possible.
It’s not just surgeons. Remember the cardiology example from above? They were generating high cost office visits and they owned the sestamibi machine. It’s not a leap to understand why they wanted all patients to get sestamibi stress tests.
Even PCPs are doing this. I can give you examples of PCPs who buy machines (X-ray, lab, etc.), even including CT scanners, which they over-utilize to make a profit. Or they have incorporated services like Physical Therapy into their office environment and refer their patients to these services.
This is all over-treatment. And about the money.
The bottom line is, the pundits like Berwick and Hackbarth, the administrators and the Finance folks make mitigating overtreatment seem simple when it isn’t. And I’m only scratching the surface with the above reasons. It is really complex.
There’s a new reliance on the Electronic Medical Record. They put in “alerts” that pop up to ask practitioners if the test or treatment is really necessary, sometimes even summarizing the literature. But there is this phenomenon called “alert fatigue” where practitioners ignore them after a while. So there hasn’t been a major improvement through the use of the EMR.
There is one article where a medical group placed alerts in the EMR and they gave practitioners a monthly report on their antibiotic use for colds. They saw a 30% reduction in antibiotic use for patients with a diagnosis of a cold (now, you have to be a little careful with data like this because all a practitioner has to do is change the diagnosis code from “cold” to something bacterial sounding to get a reduction in inappropriate antibiotic use but the actual reality remains the same) for three years. They decided that was long enough to instill a permanent change in thinking in the practitioners’ minds so they stopped the reporting. Eighteen months later, the inappropriate antibiotic prescribing rates were back to before the interventions (alerts and reports) started. This suggests getting a permanent change is complex.
The latest effort by the physician community is a program called Choosing Wisely. In truth, the recommendations make sense to the extent the “science” seems to support them. At the same time, at least 80% of the recommendations, which are listed out as recommendations by specialty, do not affect the practices of those specialties who suggested the list. For example, a procedural society recommends not doing tests or x-rays related to procedures they do, but, with some exceptions, they don’t tell their colleagues to not do their own procedures. In other words, the reduction in utilization affects another specialty or ancillary service, not their own pocketbook. Skeptical about this assessment? Here’s just a few examples pulled directly out of the Choosing Wisely list:
American Association of Neurological Surgeons
Don’t administer steroids after severe traumatic brain injury.
Don’t obtain imaging (plain radiographs, magnetic resonance imaging, computed tomography [CT], or other advanced imaging) of the spine in patients with non-specific acute low back pain and without red flags.
Don’t routinely obtain CT scanning of children with mild head injuries.
Don’t routinely screen for brain aneurysms in asymptomatic patients without a family or personal history of brain aneurysms, subarachnoid hemorrhage (SAH) or genetic disorders that may predispose to aneurysm formation.
Don’t routinely use seizure prophylaxis in patients following ischemic stroke.
None of the above affects a neurosurgeon’s revenue.
American Academy of Ophthalmology
Don’t perform preoperative medical tests for eye surgery unless there are specific medical indications.
Don’t routinely order imaging tests for patients without symptoms or signs of significant eye disease.
Don’t order antibiotics for adenoviral conjunctivitis (pink eye).
Don’t routinely provide antibiotics before or after intravitreal injections.
Don’t place punctal plugs for mild dry eye before trying other medical treatments. (This is the only one that affects an Ophthalmologists revenue)
American Academy of Otolaryngology —Head and Neck Surgery Foundation
Don’t order computed tomography (CT) scan of the head/brain for sudden hearing loss.
Don’t prescribe oral antibiotics for uncomplicated acute tympanostomy tube otorrhea.
Don’t prescribe oral antibiotics for uncomplicated acute external otitis.
Don’t routinely obtain radiographic imaging for patients who meet diagnostic criteria for uncomplicated acute rhinosinusitis.
Don’t obtain computed tomography (CT) or magnetic resonance imaging (MRI) in patients with a primary complaint of hoarseness prior to examining the larynx.
None of the above affects a Otolaryngologist’s revenue.
American College of Chest Physicians/American Thoracic Society
Don’t perform computed tomography (CT) surveillance for evaluation of indeterminate pulmonary nodules at more frequent intervals or for a longer period of time than recommended by established guidelines.
Don’t routinely offer pharmacologic treatment with advanced vasoactive agents approved only for the management of pulmonary arterial hypertension to patients with pulmonary hypertension resulting from left heart disease or hypoxemic lung diseases (Groups II or III pulmonary hypertension).
For patients recently discharged on supplemental home oxygen following hospitalization for an acute illness, don’t renew the prescription without assessing the patient for ongoing hypoxemia.
For patients recently discharged on supplemental home oxygen following hospitalization for an acute illness, don’t renew the prescription without assessing the patient for ongoing hypoxemia.
Don’t perform CT screening for lung cancer among patients at low risk for lung cancer.
None of the above affects a Chest Physician’s revenue.
American College of Surgeons
Don’t perform axillary lymph node dissection for clinical stages I and II breast cancer with clinically negative lymph nodes without attempting sentinel node biopsy. (This is the only one that affects a surgeon’s revenue)
Avoid the routine use of “whole-body” diagnostic computed tomography (CT) scanning in patients with minor or single system trauma.
Avoid colorectal cancer screening tests on asymptomatic patients with a life expectancy of less than 10 years and no family or personal history of colorectal neoplasia.
Avoid admission or preoperative chest X rays for ambulatory patients with unremarkable history and physical exam.
Don’t do computed tomography (CT) for the evaluation of suspected appendicitis in children until after ultrasound has been considered as an option.
So, only 2/25 recommendations above actually affects the specialists’ revenue, or 8% of recommendations for these five specialties.
Get the point? You don’t see these guys telling themselves to reduce or stop doing procedures they do. It’s usually someone else’s services.
But, then again, it’s all about the money.
OK, enough for now, this is getting way too long. See you in the next post!